Day(s) in the Life of...
Cameron Brady, Master of Science student
in the Cardiovascular Perfusion Program
Photos by: Kim Raff
6:00 a.m.
Four years of college basketball instilled in me an appreciation for grit and hard work. Morning hoops is where I simplify life, destress, and reset for days when I am in the OR.
6:00 a.m.
“AM Hoop Group” is more than a group of guys putting a ball through a net. It is a community of men who encourage and support each other. The group is composed of former pros, businessowners, coaches, leaders—men from all walks of life. We connect, heal, and have fun doing something we love—often without saying many words.
6:30 a.m.
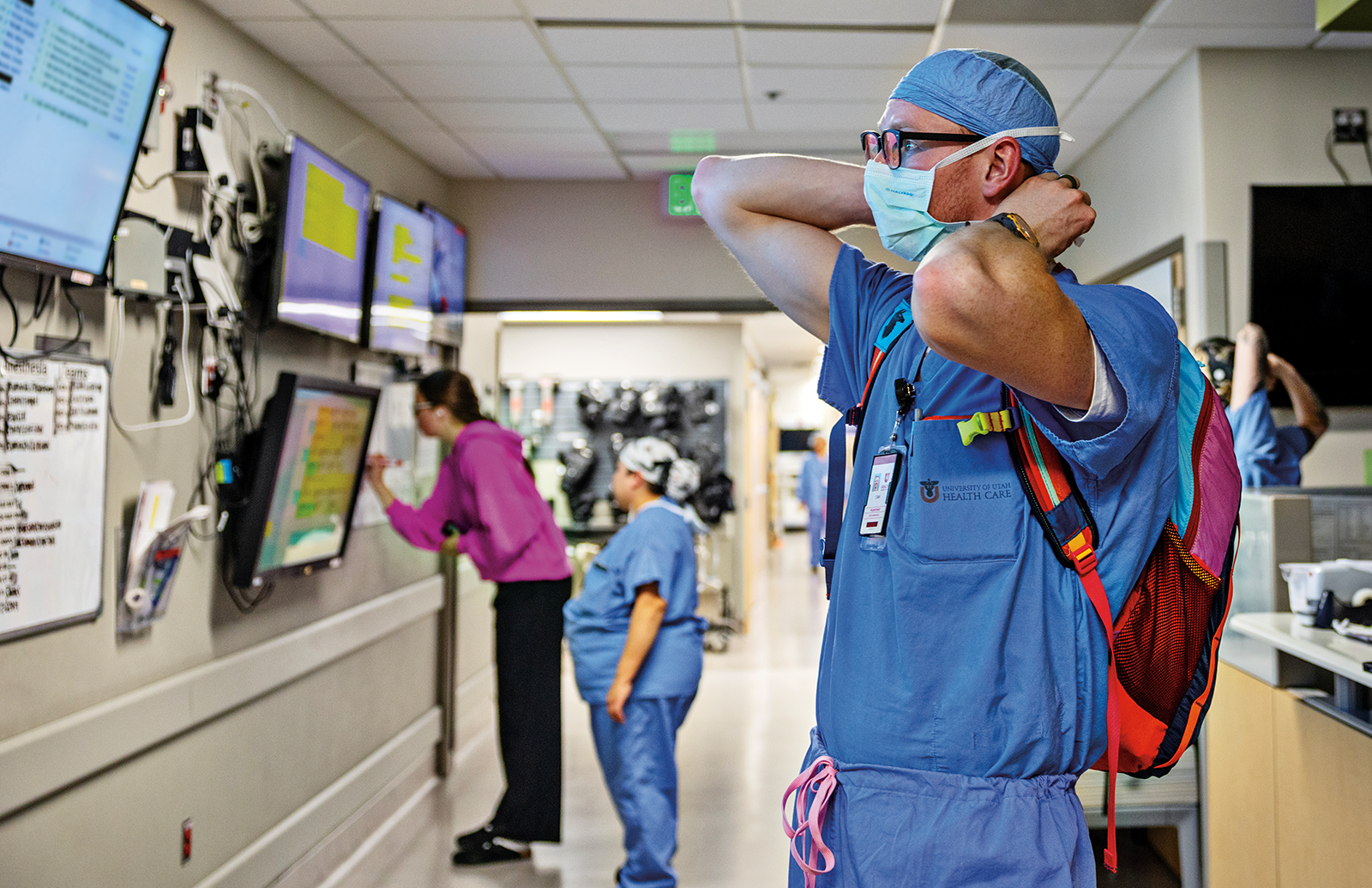
Before heading into the surgical unit, I change into the university’s blue scrubs and surgical booties, put on a surgical cap, and tie on a surgical mask.
6:40 a.m.
Ready for the OR, I review the procedure and the members of the surgical team. Understanding the different personalities of team members helps to improve team function and communication. Being cohesive as a group greatly strengthens decision making during critical moments.
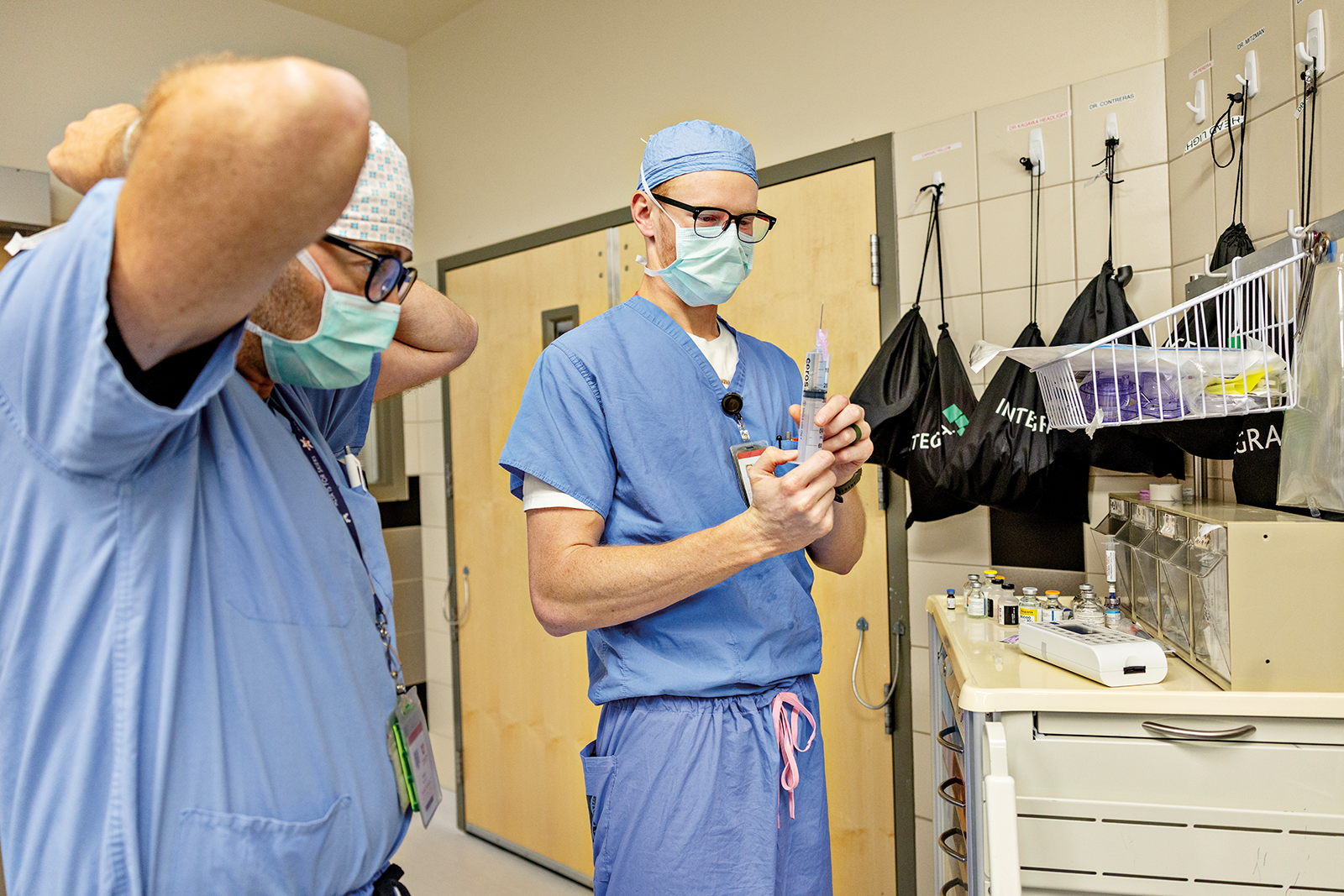
6:45 a.m.
I gather equipment and medications for cardiopulmonary bypass. As a perfusionist, I am responsible for the patient’s hemodynamic stability, blood chemistry, and safe cardiac arrest during surgery. Perfusionists use advanced medical equipment to monitor and assist in clinical decision making for each aspect of patient care throughout bypass.
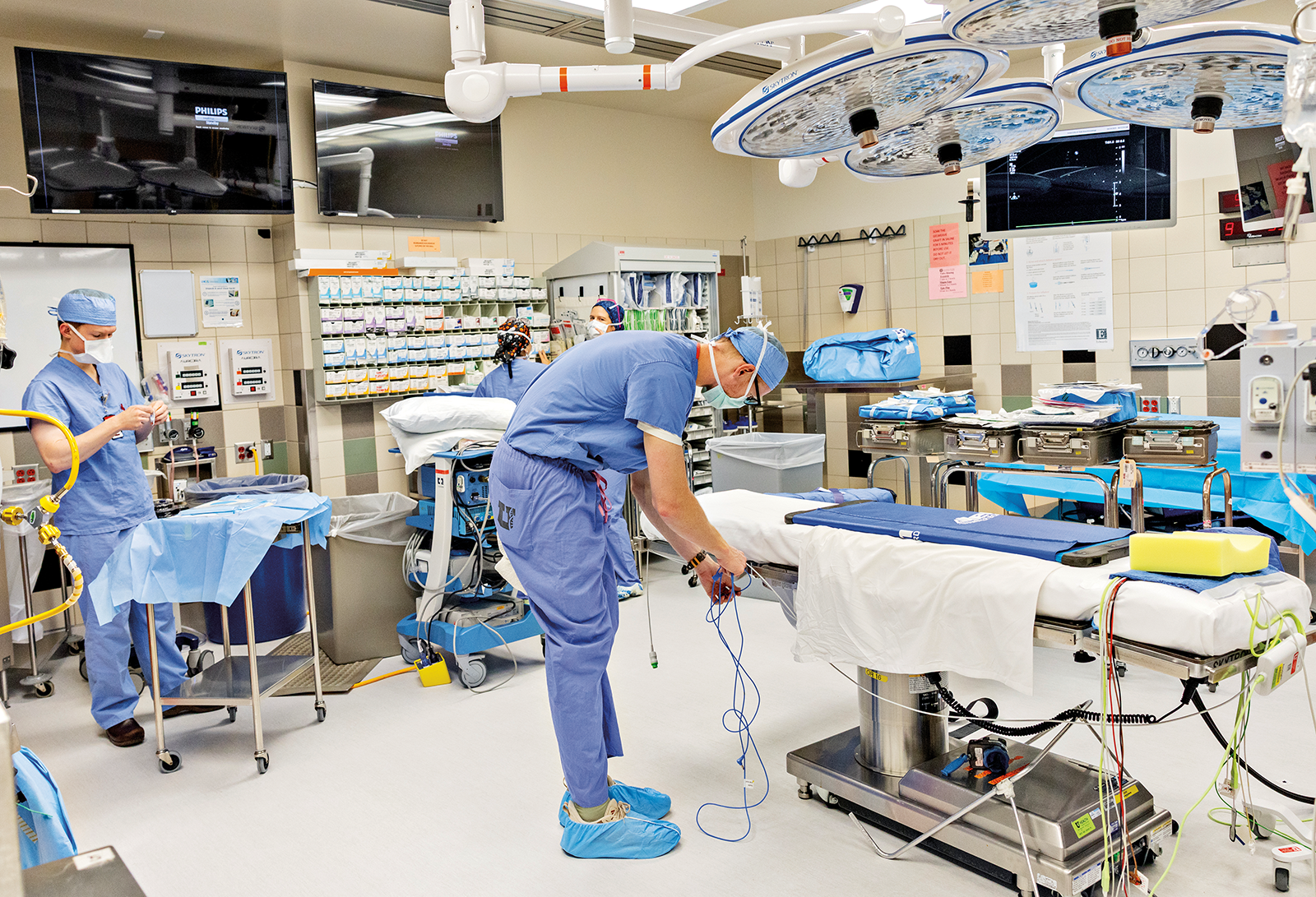
7:00 a.m.
I begin setting up the OR and preparing for the patient to enter the room. My philosophy is to be 100% ready for bypass when the patient arrives. Sometimes, our patients are very ill and require a rapid response to save their lives. At the university, multiple bypass pumps are built the night before to simplify morning setup and be prepared for any emergency, any time.
9:00 a.m.
Gas exchange is the essence of perfusion. Using a cardiopulmonary bypass machine, I assume function of the heart and lungs to provide blood flow and oxygenation and to remove carbon dioxide throughout the body while the surgeon repairs the diseased portion of the patient’s heart. This blender allows me to titrate gas mixtures to the patient’s metabolic needs.
1:00 p.m.
During each case I am accompanied by a Certified Clinical Perfusionist (CCP) while I finish my clinical training. Today my mentor was Paul Matlin, an experienced perfusionist and friend. We discuss the bypass plan including cannulation strategies, pharmacological management, and potential risks for each patient on bypass.
4:00 p.m.
At the end of each day, I am blessed to come home to my wife, Syd, and daughter, Peyton. Today I finished early. We celebrated by going to one of our favorite spots: Wheeler Historic Farm. My family grounds and supports me every day during long hours of training.