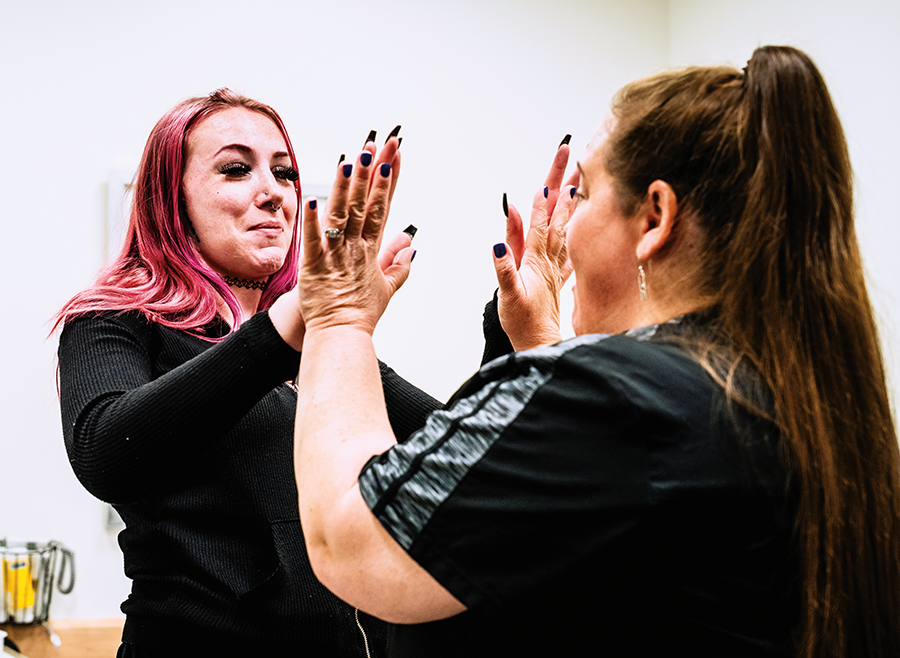Finding a Way Forward
Inside the University of Utah Health clinic, pregnancy and recovery meet—and stigma loses ground.
By: Maureen Harmon
Illustration by: Benedetta Vialli
The moment Shauna Filion tells a patient her sobriety date, the energy in the room changes: June 1, 2000.
It’s the line that divides Filion’s life in two: before and after. She doesn’t share it often. Usually, she waits until a patient looks trapped—the kind of trapped that comes from shame, or exhaustion, or both.
“If they feel stuck or like nobody understands them,” she says, “that’s when I tell them: ‘I do know how you feel. I’ve been there.’”
Filion, now the medical assistant care coordinator at the University of Utah Health’s SUPeRAD Clinic—short for Substance Use and Pregnancy, Recovery, Addiction, Dependence—celebrated her 25th year sober this summer. Around the clinic, she’s known as Mama Shauna: part confidant, part translator, part emotional first responder. Her job involves orchestrating the organized chaos: scheduling appointments, managing medications, refilling prescriptions, and supporting patients through everything from prenatal ultrasounds to insurance paperwork. But her real work happens in the pauses between those tasks, when someone needs to believe that recovery is still possible.
“I never worked in treatment before this,” she says. “But when I started at SUPeRAD, I was like, ‘This is my spot. This is my space.’”
A Clinic Built Out of Necessity
When Marcela Smid, MD, MS, MA, a maternal-fetal medicine specialist, arrived at the University of Utah a decade ago, there was no SUPeRAD. There wasn’t even a clear plan for treating substance use during pregnancy.
“No one knew what to do with patients who had opioid use disorder in pregnancy,” she says. “They’d just call psychiatry—and psych didn’t start them on medication.”
Smid, who had trained at the University of North Carolina at Chapel Hill, where the pioneering Horizons Clinic is located, was one of the few physicians certified to prescribe buprenorphine, a medication that helps people transition safely off opioids. So she taped the UNC treatment protocol to a whiteboard in the University of Utah Health clinic. “I said, ‘We do this now,’” she says. “That’s how SUPeRAD started.”
At first, it was just Smid, physician associate Jasmin Charles, MS, PA-C ’12, a small team of medical assistants, an addiction fellow, and volunteers from a campus program called Connect2Health. They opened their doors quietly—no advertising, no grant funding—just a promise to take patients, all patients.
“They came,” Smid says. “Providers started referring people they didn’t know how to help. Sisters brought sisters. A patient once told us her drug dealer wouldn’t sell to her anymore: he told her to come see us instead. That’s when we knew we’d arrived.”
SUPeRAD’s model is simple and radical: be there when people are ready. There’s a “bat phone”—a clinic cell phone carried by Filion—that rings at all hours. If a pregnant patient calls ready, she’s seen. “We never turn anyone away: we are going to meet you where you are when you are ready,” Charles says.
But sometimes, they’re not ready. “Sometimes the team meets patients in the contemplative stage, not the ready-for-recovery stage,” Charles says. “They have to find a safe place and support to get grounded before they jump in feet first for full-fledged recovery. And some of them don’t—some of them are not ready—but our doors are open.”
For those still deciding, Filion will stay on the phone for hours. Sometimes she talks to the patient’s mother, sometimes to a worried partner. “She’ll spend one to three hours with a family if that’s what it takes,” Charles says. “Because if someone’s willing to talk, that’s the window. You can’t miss it.”
“Providers started referring people they didn’t know how to help. Sisters brought sisters. A patient once told us her drug dealer wouldn’t sell to her anymore: he told her to come see us instead. That’s when we knew we’d arrived.
Once they arrive, patients are met by a four-pillar team approach: medical care, research, education, and advocacy. The clinic doesn’t run group therapy or 12-step meetings—it’s a medical space, not a treatment center—but its staff coordinate directly with local recovery programs and peer-support specialists who walk patients through everything from court appointments to child-care logistics.
They also distribute hundreds of doses of Narcan, the opioid-overdose reversal drug, and teach patients and families how to use it. “Harm reduction is a part of what we do,” Charles says. “If someone’s not in the headspace for full-fledged recovery, we meet them where they’re at, giving them a safe space and one more day to find love for themselves. We can’t support and help people when they are no longer alive.”
The ribbon is cut to celebrate the opening of the SUPeRAD clinic at the Population Health Center.
SUPeRAD patient Kelsie Buchanan holds her child as she speaks at the ribbon-cutting event.
The Uncomfortable Work of Good Medicine
Smid says addiction medicine reminds her of obstetrics: organized chaos, full of gray areas and high stakes. “You have to be comfortable with discomfort,” she says. “When I train new providers, I tell them, ‘Comfort isn’t the goal. The goal is good medicine.’”
When she started medical school at the University of California, San Francisco, in 2003, addiction wasn’t part of the curriculum. Even during residency in Chicago, it came up only as a legal issue: when to call Child Protective Services, when to detox. “That was it,” she says. “Nobody talked about it as a medical condition.”
That has changed rapidly. Addiction medicine became a recognized subspecialty in 2016, and now every accredited residency must include training on substance use disorders. Smid herself became dual board certified in maternal-fetal medicine and addiction medicine.
Here at SUPeRAD, patients see a multidisciplinary team that includes a medical doctor, a physician assistant, a certified nurse midwife, and a nurse practitioner. “The U currently has a grant to mainstream substance use disorder (SUD) education in all of the medical licensure programs,” says Charles.
“What’s happened in the last decade is enormous,” Smid says. “When I got here, no one had the tools. Now it’s malpractice not to use them.”
But for all that education, nothing teaches quite
like empathy. Filion didn’t tell Smid about her own recovery until years into their work together. “She was so nervous,” Smid remembers. “I barely remember it because it wasn’t a shock. I just thought, ‘Oh, that explains why you’re so good at this.’”
Patients feel it, too. “Some of them hear about my past at the first appointment,” Filion says. “Some it takes longer. I let it happen naturally.”
Her story has become one of the clinic’s most powerful tools—not as a confession but as connection. She now speaks at conferences and state prisons, advocating for the value of peer voices in medical spaces. “It’s been amazing to watch her grow,” Smid says. “She went from being nervous to share her story to being a national speaker. She’s proving that lived experience isn’t a liability: it’s an asset.”
Shauna Filion converses with patients at the SUPeRAD clinic.
Filion buckles a baby in its carseat.
Jasmin Charles and a SUPeRAD clinic staff member catch up with a patient.
The Science of Why Pregnancy Helps––and Why Postpartum Hurts
SUPeRAD’s providers often see women achieve stability during pregnancy—only to return to use after birth. Smid explains that this pattern isn’t just emotional; it’s biological.
“Progesterone, the dominant hormone in pregnancy, actually blunts addictive cravings,” she says. “There’s solid data showing that during high-progesterone phases—like pregnancy—women have fewer addictive behaviors. When the placenta delivers, progesterone levels crash. The brain goes into withdrawal, and suddenly everything feels unbearable.”
“We tell them, ‘Call us before it gets bad. If you start to swirl the drink, call. We’ll talk about medication options; we’ll talk about supports. We want you to survive this year.’”
That biochemical shift collides with sleep deprivation, postpartum depression, and the crushing expectations of new motherhood. “You’re supposed to be happy, and instead you feel awful,” Smid says. “You love your baby, but you’re spiraling. For someone with a substance-use history, that’s the danger zone.”
That’s why SUPeRAD extends care for a full year postpartum, long after most OB clinics discharge patients. “We tell them, ‘Call us before it gets bad. If you start to swirl the drink, call. We’ll talk about medication options; we’ll talk about supports. We want you to survive this year,’” she says.
SUPeRAD patients may receive buprenorphine injections or oral medications to manage opioid withdrawal. Some take naltrexone or acamprosate for alcohol use disorder. Patients also meet with psychiatric residents, social workers, and peer counselors—all under one roof. “This clinic is built on creativity and the reduction of barriers: we may not be able to employ a psychiatrist, so we educate ourselves in mental health care and train psychiatry and triple-board residents who can offer mental health support and learn alongside our team,” says Charles. “The same goes for phlebotomy: blood draws can be triggering for our patients, so rather than having them go to the lab, we have medical assistants and nurses trained to do blood draws in clinic rooms.”
Not all of the services offered are billable, but they can be life changing, so the SUPeRAD team often applies for grants to offset costs.
Even as public attitudes shift, stigma remains a daily battle. Job applications still ask whether applicants have ever had a substance use disorder. “If I had to check that box,” Smid admits, “I wouldn’t—not if I could help it. Because it’s still seen as a liability.”
But within SUPeRAD’s walls, that narrative is changing. “Here, we see recovery as a strength,” she says. “The skills people build in surviving addiction—resilience, empathy, discipline—those are assets. The system just hasn’t caught up yet.”
“Sometimes a patient comes in and says, ‘I’m done. I can’t do this anymore,’ and I tell them, ‘You can do this. You really can. I know—because I did.’”
Jasmin Charles hugs a patient at the SUPeRAD clinic.
Shauna Filion high-fives a patient.
A Web of Care
On clinic days, the waiting room hums quietly. A toddler might stack blocks while her mother fills out forms. Down the hall, a nurse might prep a long-acting injectable for a patient.
Each person—from provider to peer-support volunteer—keeps the clinic’s rhythm steady. “We’re the brick-and-mortar piece,” Charles says. “But the real heartbeats are the patients themselves and the network: the nonprofits, harm-reduction partners, and community workers.”
There are thousands of women around the world without access to this type of care, which is where the research and education pillars come into play—transforming the gray areas of perinatal addiction and medically informed decision-making into evidence-based medicine.
The ELEVATE Maternal Health Center of Excellence is one of twelve Maternal Health Research Centers of Excellence funded by the National Institutes of Health (NIH), aimed at reducing maternal and fetal deaths. Funded by a $14 million grant from the NIH’s IMPROVE initiative, the center focuses on pregnant and postpartum women affected by substance use disorder and often collaborates with SUPeRAD. Its work centers on changing patients’ trajectories through culturally responsive care and provider education and support.
“It’s all connected,” Charles says. “You can’t separate medical care from culture and community, from basic needs and access to care.”
Back at SUPeRAD, the clinic is buzzing with learners from all medical licensures, proving that exposure to perinatal addiction can create a ripple effect of practice. Not everyone with a substance use disorder needs SUPeRAD, but everyone deserves equal access to compassionate, educated, unbiased, and non-stigmatized care.
Eight years in, SUPeRAD has become a national model for perinatal addiction care: a program built on pragmatism, compassion, resilience, and persistence. Now, the clinic hosts trainees from across the country. Its research is shaping how hospitals approach postpartum addiction risk, and its alumni—patients and staff alike—are shaping how recovery is understood.
For Filion, every day still begins with that date—June 1, 2000—but her life’s work is about everyone else’s day one.
“Sometimes a patient comes in and says, ‘I’m done. I can’t do this anymore,’” she says. “And I tell them, ‘You can do this. You really can. I know—because I did.’”
And somewhere between medicine and grace, they believe her.